Proximal humeral fracturesProximal humeral fractures (broken shoulder) are common fractures often seen in older patients with osteoporotic (weak) bone following a simple ground-level fall on an outstretched arm. However similar injuries can occur in younger patients given sufficient trauma. The nuance of these fractures in particular, is that the pattern of the break (fracture) can be quite unpredictable and can vary hugely. This makes decision making difficult because surgeons can be put in a situation whereby they are unsure of what outcome a patient will get (the prognosis).
What is the aim of treatment ?The aim of treatment, whether it be nonoperative or operative, is to get the fracture fragments to heal in as close to 'an anatomic' (natural) position as possible, whilst allowing the shoulder some early movement to try and prevent excessive stiffness.
What will be my initial treatment ?If a doctor suspects that you may have fractured (broken) your shoulder, you will be sent for an X-ray and then placed in a sling. You are then likely to be sent home from the Emergency Department and sent a clinic appointment. It is a very painful injury. The pain will be significant for about the first 3 weeks and is often accompanied by extensive bruising around the shoulder and down the arm and the arm will swell. This will settle in time but can take 4-6 weeks. It’s a good idea to remove rings from fingers early on after injury as they can be difficult to remove after a day or so and they can compromise the blood supply to your fingers. It is uncommon to get paresthesia (pins and needles sensation) in the arm or hand with this injury. Extensive bruising down the arm, even beyond the elbow, is common and can be alarming but it does settle in 2-3 weeks. The sling you are provided with may only be a pink foam sling that goes around your neck and around the wrist. This may feel like inadequate treatment of your significant injury but there is a good reason for this. By supporting the wrist and not the elbow, the action of gravity on the arm tends to pull the fracture out straight a little. This mean that by the time you attend clinic and have another X-ray, your fracture may look slightly better, and it may even mean you can avoid surgery. You may be supplied with a blue ‘polysling’ which are more substantial but don’t tend to allow gravity to ‘pull the fracture out’ quite so much. It is ok to remove the sling for short periods to wash and dress. You don’t need to wear the sling under your clothes. Feed your clothes onto your broken limb first then onto the unbroken side, with help. If even this is too painful the wear the sling under the clothes. It is better to wear the sling during the night in bed. 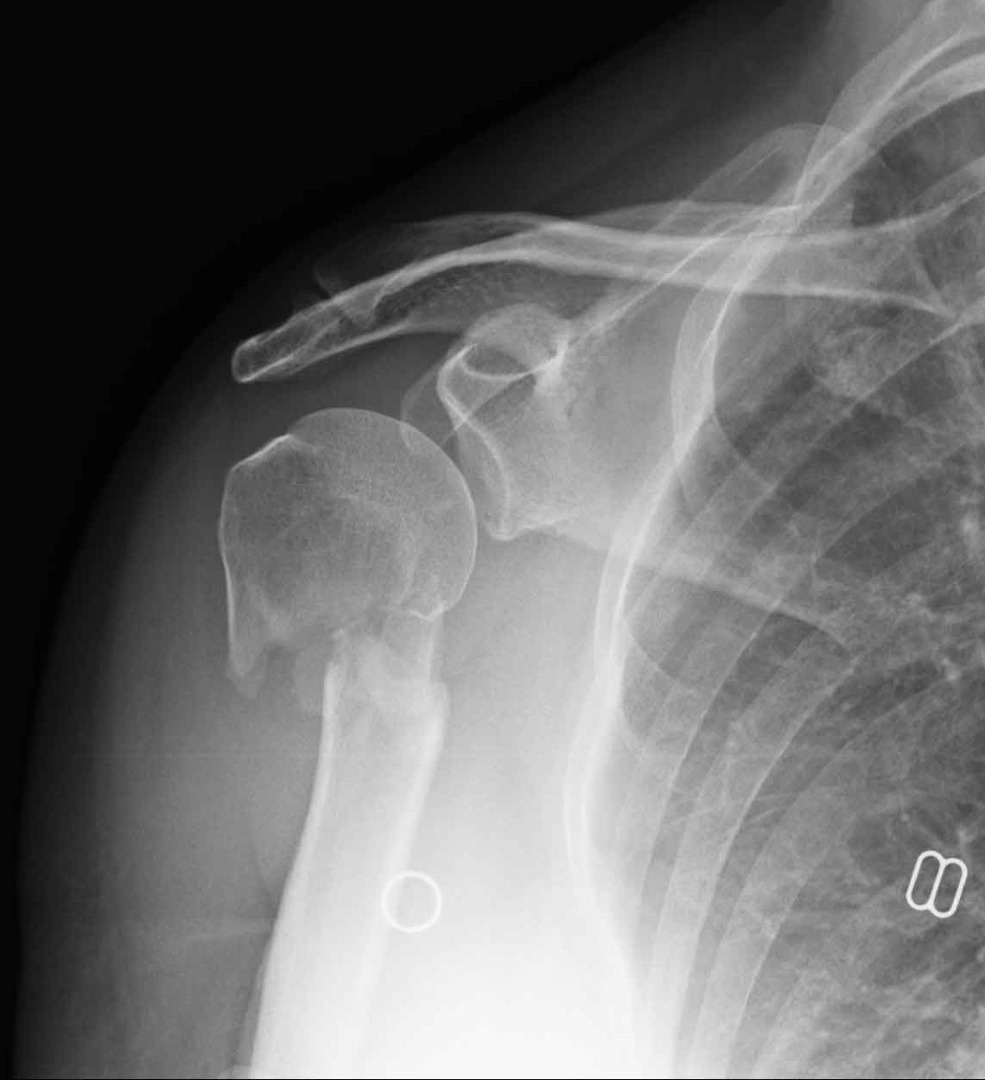
What are my options ?Once you come to clinic you will be given the chance to discuss your shoulder with a specialist in these injuries. It may be clear from your injury whether you should have a sling for a few weeks before mobilising (moving) the shoulder gradually and allowing the fracture to heal naturally (nonoperative treatment), or whether surgery is either necessary or perhaps preferable. There are really only a couple of absolute indications for surgery for this fracture. Those are open fracture (where the fracture ends have pierced the skin) or nerve or blood vessel injury. All other injuries CAN be managed without surgery, but it is a matter of what your outcome will be like. If you have complex medical problems and anaesthesia is thought to be very high risk for you then it is likely that nonoperative treatment will be preferable. This may mean accepting that your shoulder fracture should heal, but you may be left with a lot of restriction of movement. If you are young and perhaps a manual worker or a sporty-type then perhaps surgery to try and reconstruct the fracture back to something that resembles natural anatomy might be more desirable in order to stand you in the best position for movement recovery. I would say now however that some restriction, whatever the treatment, is normal following such an injury. Stiffness is a consequence of these fractures. There are ways we can try and reduce it but not eliminate it. These injuries tend to take a year to recover from, sometimes longer. 
The ProFHER TrialYou should be aware of the ProFHER Trial, the results of which were published in the medical literature in 2015. Adults with a displaced fracture of the proximal humerus were entered into the trial. At 2 and 5 years after their injury, the results of nonoperative and operative treatment were similar, indicating that there was no clear advantage to surgery. However, in reality the solution may not be that simple. The number of severely fractured (Neer 4-part) in the ProFHER trial was much lower than the 25% in the normal population, suggesting that generalisation of the results of the ProFHER trial may not be appropriate. Also, in the ProFHER study 66 surgeons operated on 125 patients over a two and a half year period, i.e., less than one patient per surgeon per year. It is hard to imagine this small proportion of patients being representative of all fractures of the proximal humeral at participating centres over this time frame. Plus, of greatest concern, there were a number of patients eligible for the ProFHER study that were excluded because they had “clear indications for surgery”. Thus, there were clearly surgeons participating in this study who felt uneasy about entering patients into a randomisation process whereby the patient may be allocated to nonoperative treatment. Intrinsically, surgeons know that a healthy 50-year-old patient with a severe fracture of the shoulder will do better with surgical intervention so bias entered the study. Lastly, there is significant residual disability and risk for complications in both operative and non-operative groups. There is clearly room for improvement. It may well be that improved implant designs or surgical techniques can enhance outcomes and justify surgical intervention for a greater proportion of patients. In addition, the standardisation of fracture pattern classification will help clarify an evidence-based approach to these patients. Thus, whilst there is evidence suggesting that fractures of the proximal humerus may be treated effectively with conservative (nonoperative) management, it is more likely that there are specific groups of patients that may indeed do better from either nonoperative or operative treatment. Currently, it perhaps isn’t as clear as we had thought. The focus on specific fracture configurations and surgical techniques may need to be at the centre of future high-quality randomised trials, which will help determine ‘on whom to operate’, and not simply ‘to operate or not to operate’. There is currently ProFHER 2 trial underway. This is to try and establish the role of reverse shoulder arthroplasty (shoulder replacement) in the treatment of shoulder fractures.  
Nonoperative treatmentShould you decide on nonoperative (no surgery) treatment, you would usually be advised to wear the sling for about 3 weeks, day and night. At about that time the fracture starts to get ‘sticky’ and solid enough to start moving it a little. This is accompanied by a improvement in your pain, indeed it is because the fracture is getting sticky that your pain starts to subside. Between 3 and 6 weeks movement forwards, backwards and to the side should become increasingly easy but no movement above the level of the shoulder will not yet be feasible. Beyond 6 weeks a physiotherapist should be assigned to you to assist your rehabilitation to try and achieve the best movement that your injury will allow. Some restriction of movement in the longterm, unfortunately, is to be expected. Final outcome is guarded until at least one year after the injury.
Operative treatmentThe two main options for fixation are a nail or a plate. The pattern of your fracture will dictate which you are offered. A nail is a titanium rod (see x-ray to the right) which is 8mm thick and about 15cm long is inserted through a small cut on the corner of your shoulder at the top and pushed down through the centre of the bone towards the elbow. There are 2 or 3 other small cuts to insert locking screws which stop the nail twisting inside the bone. The other method is plating (see lower image on the right) which is where a stainless steel plate, shaped a little like a tennis racquet, is attached to the bone with 7 or 8 screws. In hospital this may be referred to as ORIF (open reduction and internal fixation). Routinely, metalwork is left in-situ even though once the fracture has healed, the metalwork is redundant. To have the metalwork removed would be another operation which is another anaesthetic and further surgery which would be yet another opportunity to pick-up a complication and metalwork doesn’t usually provide any long-standing issues by being left in the body. Yes, you may set off alarms at airports but you’ll be able to provide a simple explanation ! Of course, sometimes it is necessary to remove metalwork if, for example, it works loose, is prominent or gets infected. These fractures are best treated with surgery, if that is the chosen treatment, within the first 3 weeks. After that the fracture is healing to an extent where the surgeon has to breakdown that healing in order to realign the fragments. This is hard work and makes the surgery longer and much more complex. Usually we would be able to arrange your surgery within 3 weeks of your injury date. You should be aware that not all orthopaedic surgeons perform such surgery so you may be waiting for a specific surgeon to have a place on his or her operating list in order to be able to get it done. This is easier said than done with pressures on our health services the way they are. You will usually come to the hospital on the day of your surgery and meet the surgeon and anaesthetist. They will re-explain the surgery and can answer any questions that you may have. The anaesthetist may offer you a ‘nerve-block’, in addition to a general anaesthetic, to assist with post-operative pain relief. The surgery usually takes between 1 and 2 hours and then you will spend some time in the ‘recovery’ area of theatres before returning to the ward. It would be usually for the operating surgeon or a member of the team to see you after the surgery to explain what went on. You may be discharged the same day or perhaps the next day, most often depending on your own home circumstances. You should wear the sling as directed, day and night but it can be removed under certain circumstances and this is not detrimental to your surgery. You can remove it to get washed or showered. You may need help. Keep your arm in the position that it would be if it were in a sling (forearm across your tummy) and hold the shower-head in the other hand. Shower low-down, using only a flannel near your dressing and into the armpit of the operated arm. Do not get your dressing wet. If it gets wet, it needs changing and the more a dressing is changed the more likely the wound will get infected. It is also ok to remove the sling to do some gentle exercises of the elbow to avoid stiffness and of course the hand and wrist. The physiotherapist on the ward will show you some gentle exercises to do for your shoulder also. At about 2 weeks after your operation you will come back to the hospital to have you wound checked and any stitches trimmed or removed. After this it is common to be able to get the wound wet in the shower. Be gentle with the wound as it is still fragile. Don’t rub it vigorously with a towel but dab it dry. Be gentle with the wound for 6 weeks after the operation. I would usually recommend a patient to use a sling for about 4 weeks after fixation of a shoulder fracture. After 4 weeks start to move your shoulder through a gentle range, initially moving the arm below the level of the shoulder and increasing to above the shoulder after a couple of weeks but the physio will advise you. All patients progress slightly differently. Some pain is to be expected. It can be difficult for patients to know how much physio to do and what it should feel like both during and after doing the exercises. If you don’t do enough then obviously it won’t be beneficial. If you do too much then you may get a lot of pain and even do damage to the surgical repair. As a guide, you should have pain for no longer than an hour after doing your exercises. If you’re pain is lasting longer than this, you may be doing too much. The pain you experience during the exercises should not go above 5 on the pain scale (1-10, with 10 being the worst pain imaginable). If your pain does go above this level then you need some gentler exercises to work with initially before building back up. You will be reviewed again at about the 2 month mark. By this time your pain should be under control, you should be getting well on physio. Driving is feasible at about this stage for many. Patients that drive cars with automatic gear-boxes tend to get back into driving much sooner than those with manual gearboxes, especially when it’s the left shoulder that was fractured. The DVLA just advise no plaster casts and no slings. After that it is down to the driver to declare for themselves whether they feel safe to drive. You will be followed-up in clinic for as long as it takes to see that your injury has recovered to a satisfactory level. X-rays may be taken to check the healing position.
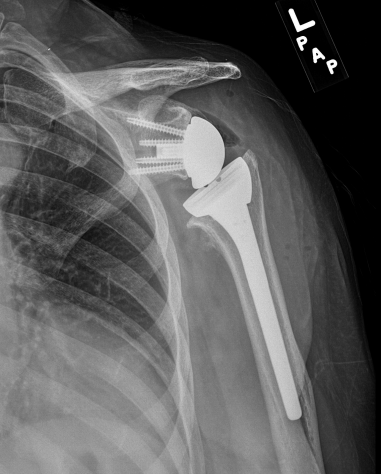 What about shoulder replacement ?If your fracture is severe there may be no realistic chance of piecing the fragments back together and it may be recommended that you have a total shoulder replacement. This would be in the form of a reverse shoulder replacement (RSA). This is named this way because the ball and socket components are switched around so the socket sits at the top of the humerus (the arm) and the ball (half of a ball) sits on the shoulder blade. The reason for this is that the main tendons in the shoulder will no longer function properly due to the fracture. In order to make the most of your only remaining good muscle (deltoid), the centre of rotation of the shoulder is changed by reversing the way the joint works. Your shoulder looks the same form the outside. Unfortunately if you have gone from a normal shoulder one day to then having a fracture and then having a RSA, you are not likely to think that an RSA feels ‘normal’. However, it shouldn’t feel painful and this will give you the best chance, under the circumstances, of lifting your arm up again.
Isolated greater tuberosity fracturesIt is possible to just break the greater tuberoisty (the corner) from the shoulder (proximal humerus). This is commonly associated with an anterior dislocation of the shoulder in patients over 40 years of age. Whilst the fracture fragment may look small it is a very important because the rotator cuff (main tendon to lift the arm up) is attached to the great tuberosity. it is therefore important to make sure the fragment heals in the correct place. Due to the pull of the tendon (and the muscle), the fragment commonly displaces (moves) posteriorly. If it heals here then shoulder movement will be hugely compromised. The normal stabilising force of the rotator cuff is lost and the shoulder will feel weak and painful.
The method I employ for re-attaching these fragments is via an open approach (not arthroscopic). The cut is on the side of the shoulder and I define the fragment in the space just above the shoulder. I then use a combination of strong sutures (stiches) between the bone and the tendon to pull the fragment back to where it should be. I use anchors into the bone to hold the stitches in place. Using metal screws in this situation is usually very disappointing. The bone quality here is usually poor so the screws just pull out, if not actually during the operation then shortly after ! The tendon however is usually very strong and so that is where the hold is best.
I usually ask a patient to wear a sling for about 4-6 weeks after the surgery to allow the tendon to heal into place. Gentle, early movement from day 1 is allowed however, under the guidance of a physiotherapist. Even with reconstruction of the bone and tendon back into position, patients often experience significant stiffness and regular and intense reabilitation with a physiotherapist is essential afterwards to regain a good range of movement of the shoudler. 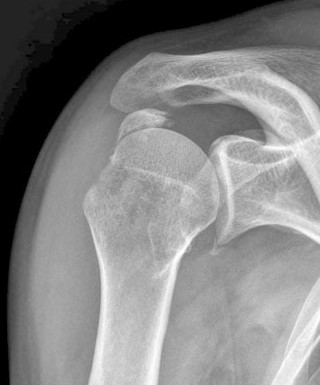
|